|
India
representing one sixth of humanity with the maximum number of two
wheelers is a paradox. State of the art neuro intensive care units and
teleconsultation through VSAT satellites exist, along with poor
infrastructural facilities. A fatality every four minutes makes head
injury the sixth commonest cause of death. Only 800 neurosurgeons are
available for a population of 1050 million. 25000 million rupees 1% of
the GDP of India) is the annual loss due to road traffic accidents alone.
70% of head injuries are preventable, occurring due to negligence and
ignorance. Less than 5% of all head injuries require surgical
intervention.
A
significant number of head injuries present with primary or secondary
injuries in and around the globe of the eye. These patients may initially
present to an ophthalmologist .Optic Nerve damage in closed head injury
occurs in 0.5-3% of all head injuries. The actual injury to
the head is often surprisingly mild and at times the patient may not even
be concussed. The true incidence of post traumatic visual problems may be
higher than generally believed. Bilateral optic nerve injury is much less
frequent than unilateral injury. Hippocrates described optic nerve
injuries in ‘De Morbis Vulgaribus’ as early as 1200 B.C as
“Dimness of vision occurs in injuries to brow and in those placed
slightly above it” Any update on neuro-ophthalmology should therefore
include a discussion on head trauma and its effects on the visual system.
Clinical
evaluation in head injury:
Circumstances
surrounding trauma usually preclude a detailed neurological examination,
especially the need to triage multiple injuries and the lack of patient
cooperation. This leads to an abbreviated evaluation but one that
can be repeated frequently to observe improvement or deterioration. The
initial neurological examination frequently leads to a conclusion of
either focal or non-focal changes. History of alcohol consumption
confounds the situation. Head injury is so obvious, that a complete and
detailed history is sometimes not taken. This is particularly
important with reference to the visual status. Failure to record the
history on admission may result in loss of the only opportunity to get
this valuable information from ambulance drivers, the accompanying
bystanders and police officers.
It
is specially important to record the nature of the accident, the interval
between injury and examination, history of convulsions after injury,
state of consciousness from the moment of injury till the time of
examination, history of any drugs administered prior to admission and
history of any significant concurrent or past illness (diabetes,
hypertension, ischaemic heart disease). History of the use of miotics or
mydriatics, previous ophthalmic surgery may not be immediately available
particularly if the patient is unconscious.
Cranial
nerve function can be clinically evaluated even in a stuporous or
comatose patient : this helps assess functioning of the brain stem as
well.
|
The pupillary light reflex
requires the afferent link of the optic nerves and tracts to be intact
as well as the parasympathetic oculomotor outflow for the efferent
link.
If
the cervical spine is not injured extra ocular movements may be tested
by rotating the head in various directions. The globes will be
fixed at a particular point in space, regardless of head rotation, and
the eyes kept passively at a certain gaze if the “doll’s eye” response
|

|
|
(oculocephalic reflex) is
preserved. The extraocular muscles also receive a strong input
from the vestibular system. Caloric testing of labyrinthine function
also tests the efferent eye yoking
|
direct external injury to the eyes
|
|
responses, assuming that the
vestibular system is intact. Vestibulo-ocular reflex is elicited by
caloric assuming that the vestibular system is intact. Vestibulo-ocular
reflex is elicited by caloricstimulation of the labyrinth. Normally
on irrigating the external ear with cold or warm water, nystagamus
can be observed if the brainstem is intact.
|

|
|
In comatose patients
evaluation of the vestibulo-ocular reflex can provide valuable
informationregarding the integrity of the vestibulo-ocular pathways
which traverse the
|
Subconjunctival hemorrhage with fracture
orbit.
|
|
brainstem. It is
possible to evaluate the abnormalities of ocular nerves or gaze
paralysis. In addition, it helps in prognostication. If the
vestibulo-ocular reflex is not elicited, brainstem dysfunction can be
inferred.
|

|
|
For the direct light reflex
to be present, the mesencephalon must be functionally preserved, while
the oculocephalic and caloric responses require the medulla and pons
also to be
|
Posttraumatic Carotico Cavernous Fistula
|
functioning.
The light reflex in particular is an excellent index of midbrain
function, assuming that the afferent arc is intact. The pupillary
fibres in the third nerve may also be compressed in the transtentorial
herniation syndrome, leading to dilatation due to the external location
of these fibers on the surface of the nerve. The size of the pupils
in millimeters, and their reaction to light both direct and consensual
should be recorded. Evidence of local injury to the eye, the
margins of the iris and fundus findings should be documented.
The
pupillary size depends on the equilibrium between parasympathetic
constriction and sympathetic dilatation. Recording of pupillary
status and its changes gives information about the upper brainstem, the
third nerve and the second nerve. The afferent pathway for the
pupillary reflex is through the retina and the optic nerve. The
efferent pathway is through the third nerve. Thus a study of the
direct and consensual light reflexes helps to distinguish between second
and third nerve injuries.
Unilateral
miosis can occur in cervical sympathetic paralysis (Horner’s
syndrome). This can be seen in injury to the carotid artery.
The
contralateral pupil may appear bigger and one should not mistake it for a
3rd nerve deficit.
Bilaterally
dilated pupils indicate a bad prognosis. However bilateral glaucoma
with blindness, parenteral administration of atropine or its local
instillation, or poisoning with dathura and gluterthamide may lead to
pupillary dilatation.
Irregular
pupils can be seen in patients with accidental or post surgical aphakia
and after cataract extraction. In opiate or barbiturate poisoning,
miosis is observed.
Coloboma
of the iris is seen as a defect in the iris at about six ‘o clock
position and the pupils are irregular. This should not be mistaken
for a unilateral dilated pupil indicating an intracranial hematomas.
With
light thrown into a blind eye, the direct reflex is lost in both the eyes
while the consensual reflex is preserved. If there is a hemianopia,
such a sign can be elicited from the blind side of the eye.
Gaze
palsies can occur following head injury. Upward or downward gaze
palsies as well as lateral conjugate gaze palsies could occur. At
times skew deviation may also be noted.
The
fifth cranial nerve may be involved in middle cranial fossa
fractures. Fractures of the middle fossa involving the
petrous-pyramid can manifest with CSF otorrhoea, lower motor neuron
facial palsy, deafness or vertigo. Facial palsy may recover but
deafness usually persists. The trigeminal and facial nerves may be tested
with corneal responses to a light cotton wisp or response to more severe
facial stimuli, to assess for facial grimace and eye closure.
Pupils
not reacting to light on both sides, with absent oculo vestibular
reflexes, in deeply comatose aresponsive apnoeic patients, with severe
brain injury, are a clinical sign of brain death and should not be
attributed to bilateral optic or 3rd nerve injury.
Bilateral
small pupils may occur as a result of pontine hemorrhage due to
interruption of diencephalic and reticular inhibitory influences on the
Edinger-Westphal nucleus.
A
unilateral contracted pupil with the retention of the light reflex may be
due to interruption of the sympathetic pathways in the brainstem,
cervical spinal cord, or neck.
Eccentric
pupils have also been seen in midbrain injuries and are associated with a
poor prognosis. The pupil may also be involved in direct injuries
to the eye. This usually manifests as a dilated irregular pupil,
reacting sluggishly to light.
A
dilated pupil due to cerebral herniation may revert to normal size once
the compression is relieved. However, a dilated pupil due to injury
to the oculomotor nerve may take a long time to recover and sometimes may
not recover.
The
most common form of trigeminal nerve injury after head trauma involves
the supraorbital and supratrochlear nerves as they emerge from the
supraorbital notch and superomedial aspect of the bony orbit.
Branches of these nerves may be contused or divided, resulting in
anesthesia of a portion of the nose, eyebrow, and forehead extending as
far back as the front of the ear.
A) Optic nerve injuries:
The optic nerve is a tract consisting mainly of the axons of
the ganglion cells of the retina . These axons converge on the optic
disc, which is approximately 1.5mm in diameter, pierce the sclera at the
lamina cribosa, a sieve-like structure, then form bundles of myelinated
nerve fibers separated by connective tissue septa. Largely because of the
presence of the myelin sheaths and the connective tissue septa behind the
level of the lamina cribosa, the optic nerve has a greater diameter at
the point at which it leaves the globe than at it's head (the optic
disc).
Each optic nerve is encased in sheaths continuous with and
similar to the meninges of the cranium (pia, arachnoid, and the dura).
Blood supply: The
arterial supply to the optic nerve anterior to the lamina cribosa is
derived from the short ciliary arteries. Immediately behind the lamina
cribosa vessels derived from the Circle of Zinn, which is itself supplied
by the short ciliary arteries, enter the optic nerve. The orbital portion
of the optic nerve derives its blood supply from the pial circulation and
perhaps also to some extent from the ophthalmic artery and its branches,
including the central retinal artery. That portion of the optic nerve
lying in the optic canal derives its arterial blood supply from the
ophthalmic artery, whilst the intra-cranial part of the optic nerve is
supplied centripetally through the pial vessels. Venous drainage from the
ocular and orbital portions of the optic nerve is chiefly into the
central retinal vein.
The optic nerve may be considered as consisting of four
parts:
1.Intraocular (1mm ) segment is the head &
ocular portion which traverses the sclera and subject to avulsion injuries.
The optic nerve head will not be seen ophthlmoscopically. Hemorrhages may
be seen around it. The optic nerve head will not be seen
ophthalmoscopically
Due to the cushioning effect of the structures in the globe,
this part of the nerve is least prone for injury.
2.Intraorbital (23mm to 30mm ) is the longest.
It is sinuous to enable the movement of the eye ball. Intra orbital
hemorrhage can cause compressive optic neuropathy with proptosis and
elevated introcular pressure. The nerve sheath can also contain
a hematoma.
3.Intracanalicular ( 8mm ) is fixed within
the long optic canal. The optic nerves are often damaged most severely
just adjacent to or within the optic canal. The firm attachment of the
dural sheath to the optic nerve makes it particularly susceptible
to shearing, stretching or torsional forces, compression by fracture ,
hemorrhage , edema and/or ischaemia.
4.Intracranial (15mm ) extends from the optic canal
to the anterior part of the optic chiasm.
Clinical
features:
·
Optic nerve injuries may be overlooked initially in patients with severe
concomitant head or eye injuries.
·
Optic nerve injury presents as loss of vision in the affected eye
with a dilated pupil
·
Affected eye reacts to consensual light but not to direct light ( Marcus
Gunn pupil)
· There
may be no evidence of external or internal injury or there may be
bruising around the eye because of the frontal nature of the injury or
proptosis due to associated retro-ocular swelling and bleeding
·
No fundus changes may be apparent initially though optic disc pallor/
atrophy may set in 4-6 weeks later.
·
In case of anterior marginal tear there may be edema and retinal
hemorrhage.
·
External injury may make it difficult to determine the exact cause of
blindness
·
Most often the head injury is very minor with no significant loss of
consciousness.
·
In unconscious patients the diagnosis of optic nerve injury is made only
on pupillary findings and confirmation of diagnosis is only possible by
VEP
·
The severity of the external impact has no correlation with the degree of
visual loss.
·
Various types of field defects can occur
·
Damage to optic radiation optic tract or geniculate body is difficult to
diagnose clinically in unconscious patients
·
In unconscious patients with both 2nd and 3rd nerve
involvement in the same eye, diagnosis can only be established by VEP
·
In spite of immediate loss of vision in one eye the patient may not
complain of blindness especially if the patient is a child or is in
altered sensorium. In addition, examination of the pupils may not
show any difference in size when both the eyes are open.
·
Unilateral blindness due to optic nerve injury is often missed on a quick
clinical examination in the emergency room. However, careful
neurological testing will reveal the visual loss. The pupil on the
affected side dilates when the opposite eye is closed. In addition,
light thrown into the affected eye does not cause constriction of the
opposite pupil. These findings help to differentiate, even in an
unconscious patient, unilateral optic nerve injury from other causes of
unilateral enlarged pupil.
·
Other causes of dilated pupils include traumatic mydriasis due to injury
to the optic chiasma or the oculomotor nerve, as well as primary
brainstem injury. In traumatic mydriasis, careful examination,
preferably with a loupe or a powerful magnifying glass, shows
irregularity of the margin of the pupillary aperture.
· In
oculomotor nerve palsy both direct and consensual light reflexes are lost
in the same eye, while in optochiasmal injury the opposite pupil also
shows a sluggish reaction to light.
· In
injuries to the brainstem, the pupils show frequent variations in size
when observed over a period of time and there are other associated
features like altered vital signs, alteration in tone of the limb
muscles, conjugate palsy and nystagmus.
·
Some patients show delayed visual loss. These patients have normal
vision immediately following trauma .Progressive deterioration of vision
occurs later. It is possible that the delayed type of deterioration is
merely a progression due to increasing edema of a partial lesion which
occurred at the time of the impact.
·
Papilloedema may rarely be seen following optic nerve injuries, and is
often accompanied by contraction of the visual fields. Sooner or
later, however, changes of primary optic atrophy set in. After a
few days, a squint of the blind eye becomes obvious, as it assumes a
neutral position (as if looking straight ahead) due to the loss of
visually mediated muscle tone. The normal eye continues to maintain
the normal position of slight inward tilt.
·
Field defects reported include bi temporal hemianopia central and
paracentral scotomas and altitudinal hemianopia.
·
Rarely a patient with an undetected sellar or suprasellar lesion may
sustain a minor head injury. The pre-existing field defects may be
detected only after the injury and be mistaken as being due to chiasmal
injury.
·
Division of the optic nerve close to the globe causes interruption of the
central retinal vessels. The ophthalmoscopic picture is that of
central retinal artery occlusion; there is immediate pallor of the optic
disc, a gray retina with narrowed retinal vessels, and a cherry-red spot
at the macula. The intraocular portion of the optic nerve may be
completely or partially avulsed from the globe, producing hemorrhages at
the disc margins. These hemorrhages resorb in about two weeks,
leaving a pigmented scar.
·
Complete avulsion of the optic nerve head causes total blindness. A deep round hole may be seen on
ophthalmological examination. This cavity is filled within 2 months
by white connective tissue, and the surrounding retina develops thick
folds. Division of the optic nerve posterior to the point of
entrance of the central retinal artery produces total blindness, but
funduscopic examination is initially normal. Pallor of the optic
disc will develop in time, depending on the area of optic nerve
disruption, and occurs most promptly with injuries closest to the globe
·
With an injury to the optic nerve within the optic canal, the pallor of
the fundus is usually evident 3 weeks after injury. Injury to this part
of the optic nerve invariably occurs in association with direct trauma to
the globe as the nerve is pushed posteriorly and suffers a partial or
complete avulsion at the back end of the globe. The ophthalmoscopic
picture consists of a marginal hemorrhage extending to the disc.
The hemorrhage soon disappears, to be followed by a pigmented scar.
Concomitant intraocular hemorrhage makes funduscopic examination
unrewarding. On visual field examination, there is a sector defect
extending from the blind spot to the periphery.
·
Although fractures of the orbit are common, isolated injury to the
intraorbital portion of the optic nerve is rare .With severe trauma to
the apex of the orbit, there may be a disruption of the sphenoidal
fissure with loss of function of third, fourth and sixth nerves, and the
ophthalmic branch of the fifth nerve, accompanied by monocular blindness and
proptosis secondary to hemorrhage into the muscle cone. Under these
circumstances, a decompressive procedure through the maxillary antrum has
been described to alleviate the proptosis. The most vulnerable component
of the optic nerve in patients with head trauma is that portion of the
nerve located within the optic canal. Majority of cases follow
closed head injuries, primarily those involving frontal, temporal and
orbital regions.
·
Recovery, if any, in a case of optic nerve injury commences within a few
days of the trauma. Before vision starts to recover, return of some
pupillary function may be seen within forty-eight hours. Once
recovery starts, it may continue slowly over a period of several
months. If recovery does not begin within a few days the prognosis
is grave.
Pathophysiology
of optic nerve injuries:
Direct injuries are due to penetration of
the orbit by missiles, sharp objects or bone fragments resulting in
transection of optic nerve fibers .The entry site may be obscured by red swollen
conjunctiva. It must be carefully looked for. Optic nerve can also be
injured during various surgeries around it. Anesthetic agent can
infiltrate into the optic nerve and central nervous system accidentally,
at the time of retro bulbar injection .
Indirect injuries occur due to
transmitted forces in head injuries particularly forehead .Walsch &
Hoyt defined such an injury as traumatic loss of vision which occurs
without external or internal ophthalmoscopic evidence of injury to the
eye or its nerves.
In the
majority of instances, the pathological findings have been derived from
autopsy material on patients dying after severe cranial trauma where
there was little information regarding the visual function. Autopsy
studies indicated involvement of anterior visual pathway in
44% , 24% being bilateral.
The
pathogenesis of optic nerve injury is still debated.
In
addition to the anatomical disruption and mechanical compression due to
hematoma and edema, vascular insufficiency also plays an important role
in the resultant injury.
The
mechanism of injury may be stretch lesions tearing the fibers, injury to
the blood vessels supplying the chiasma, division of the chiasma by a
bone fragment or a hematomas in the sella turcica. In the majority
of cases, the cause is a direct tear or contusion.
The
primary lesion is rarely a total section or laceration, but is usually a
contusion, necrosis, ischemic necrosis or interstitial hemorrhage due to
a blow or shearing occurring at the moment of injury Hemorrhage in the
optic nerve sheath, complete or partial optic nerve tear,
concussion, contusion or laceration of the optic nerve and
optic canal fracture can occur. Secondary edema, ischemia and
infarction may occur due to vascular thrombosis.
Indirect
optic nerve injury due to blow over the forehead may be due to
acceleration and deceleration on the long axis of the orbit resulting in
shearing strain.
Loss of
vision after trauma may occur in consequence of direct optic nerve injury
or as a result of interference with the blood supply of the nerve.
When loss of vision occurs immediately after the trauma, it is impossible
to determine whether the optic nerve has been severed or contused, is
edematous, or is ischemic. If the loss of vision returns subsequently,
it is obvious that the optic nerve is intact and the previous visual loss
was secondary to transitory ischemia or nerve swelling with impaired
axonal conduction. Delayed loss of vision after trauma always
indicates that the optic nerve is intact, with the late visual loss being
secondary to infarction or less commonly hematomas surrounding the nerve
or to callus formation, usually within the optic canal.
Trauma
to the orbit, with or without significant craniocerebral trauma, is
rarely neatly circumscribed, and a severe injury to the eye may involve
varying admixtures of optic nerve, extra ocular muscle and nerve, and
optic globe insults. The optic nerve may be considered to have four
components: intraocular, intraorbital, intracanalicular and intracranial.
Isolated optic nerve injury occurs primarily within the bony optic canal,
which measures from 4 to 9 mm in length and 4 to 6 mm in width.
Each canal is directed posteriorly and medially from the posterior orbit.
The intracanalicular part of the optic nerve is more frequently
injured. Within the canal, the optic nerve is surrounded by
an extension of the dura mater, as well as the pia and arachnoid.
The ophthalmic artery also transverses the canal inferior and lateral to
the nerve. Sympathetic fibers from the carotid plexus en route to
the ciliary body of the pupil are also contained within the canal.
The blood supply to the intracanalicular portion of the nerve is derived
from small penetrating branches of the ophthalmic artery and a recurrent
branch of the central retinal artery that arises within the orbit and
extends back into the optic canal. The orbital portion of the optic nerve
measures 20 to 30 mm in length and extends from the anterior portion of
the optic canal to the posterior portion of the globe. It lies
rather loosely in a lazy S- shaped configuration covered by dura mater,
pia, and arachnoid. The central retinal artery and vein penetrate
the infero medial portion of the nerve almost at right angles, entering
it from 5 to 15 mm posterior to the globe. The intracranial portion of
each optic nerve is directed posteriorly and medially for a distance of 5
to 16 mm and ends where the optic chiasm is formed. The internal
carotid artery lies lateral to the optic nerve, whereas the ophthalmic
artery is usually lateral and interior to the nerve. The optic
nerves have important relationships with the sphenoid sinus, posterior
ethmoid cells, and cavernous sinuses. The arterior cerebral
arteries pass above the posterior portions of the optic chiasm, where
they generally form the anterior communicating artery.
Injury
to the posterior visual pathway occurs in severe head injuries.
Penetrating injuries may injure the optic tract, optic radiation and
calcarine cortex . In closed head injuries this may be due to contusion
or intracerebral haematoma in temporal, parietal or occipital lobes
shearing or posttraumatic thrombosis of arachnoidal vessels supplying the
central chiasma could cause chiasmal damage.
Operative
findings often reveal a grossly normal optic nerve. Rarely,
hemorrhage into the nerve sheath or within the nerve, and arachnoidal
adhesions have been reported. In spite of the normal appearance of
the nerve at the time of surgery or at autopsy, microscopic studies have
consistently demonstrated various pathological processes such as
degeneration of myelin, loss of axon, necrosis of a portion of the nerve,
and areas of chronic inflammation with phagocytosis. Evidence of
vascular involvement in the form of thrombosis, ischemia and infarction
was seen in some cases.
Depending
on the site of damage, four types of injuries can be recognized: anterior
marginal tears (12 percent), anterior optic nerve injury (14 percent),
posterior and canalicular optic nerve injury (67 percent) and
optochiasmal injuries
Anterior
marginal tear: Here
the optic nerve is injured close to the optic nerve head in the retina,
usually as the result of trauma over the forehead or over the
supraorbital area. Anterior marginal tear is likely to be
associated with retinal injury or chorio retinal injury.
Ophthalmoscopy reveals hemorrhage in the optic disc and an irregular disc
margin; the hemorrhage disappears after sometime leaving a pigmented
scar. These patients have a sectorial visual field defect from the
blind spot to the periphery.
Anterior
optic nerve injury: In this type the nerve is involved anterior to the
entry of the retinal artery and results from forehead trauma.
Ophthalmoscopy does not reveal an immediate disc abnormality.
However, fundus changes set in much earlier than in the posterior type of
optic nerve injury. The fundus reveals a pale disc with grey retina
and thinned out blood vessels. Sometimes a cherry red spot may be
seen in the macula.
Posterior
optic nerve injury: This results from injury to the optic nerve (a) in
the posterior part of the orbit, (b) in the optic canal, or (c)
intracranially. Injury to the intraorbital part is relatively rare
as the nerve is redundant and well protected by the cushioning effect of
fat and muscles. Traumatic orbital apex syndrome due to damage of
the optic nerve inside the muscle cone is a rare condition. In this
condition there is a fracture of the orbit and the intraorbital vessels
are torn leading to an intraorbital haematoma in the muscle cone which in
turn results in proptosis. The loss of vision is also associated
with involvement of the II, IV and VI cranial nerves.
Intracanalicular
involvement of the optic nerve is much more common than its involvement
at other sites. The incidence varies from 0.6 to 2.0 percent of all
head injuries.
Bilateral
injury of the optic nerve is very rare and is usually associated with a
transverse fracture of the floor of the anterior cranial fossa.
Ischaemia: In the
majority of cases, the blood supply to the optic nerve seems to be
compromised by the injury. As the nerve passes through the optic
foramen, its dural sheath is more closely adherent to the bone in its
upper part. Shearing stresses during injury appear to disrupt the
blood supply in this region easily. The frequent incidence of the
inferior hemianopic type of field defect is explained on this
basis. Transient visual loss may be due to transient vasospasm as
suggested by some authors and is termed “Optic nerve concussion”.
Rupture: Rupture of
nerve fibers occurs due to shearing or torsion. The entire nerve
may be affected or some fibers only may be ruptured resulting in a fiber
bundle type of defect in the visual field.
Compression
or Contusion: The nerve may be involved in a fracture. In rare
cases a spicule of bone may be seen to impale the nerve.
Occasionally a communited fracture may squeeze the optic foramen and
narrow it with resultant compression of the nerve. Fracture of the
optic canal produces injury in a small number of cases. Fracture of
the anterior clinoid and the orbital roof can also damage the optic
nerve. In these fractures, disruption of the continuity of the
canal with compression or tear of the nerve is likely.
Hemorrhage
into the optic nerve sheath is less common. The bleeding could be
intraneural, subarachnoid or subdural.
Intraneural hemorrhage may occur due to rupture of small veins or
capillaries resulting in a perivascular haematoma.
Investigations:
|
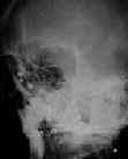
X-ray skull - optic foramen and superior orbital fissure view
and para Nasal Sinus views are essential. Soft tissue opacity and air
fluid level in the para nasal sinuses indirectly indicate a fracture
through the anterior cranial fossa. Sometimes a fracture line can
be demonstrated across the sella turcica. As this fracture may
open the sphenoid sinus, post-traumatic meningitis may result. A
plain lateral film of the skull with the patient in the sitting posture
may occasionally show a fluid level in the sphenoid sinus or air in the
chiasmatic cistern, confirming the CSF leak.
Fracture
of the roof of the optic canal with frequent extension into the roof of
the orbit has been documented. Fractures of the base of the skull may
extend into the optic canal. Whether the fracture of the optic
canal is the primary cause of the nerve injury or
|
|
|
constitutes an epiphenomenon
associated with other insults (contusion, necrosis, ischemia
|
Pellets in the orbit-Xray
|
|
and so forth) is a source of
controversy. Optic nerve injury causing blindness occurs without
a radiologically demonstrable fracture in about 20%.
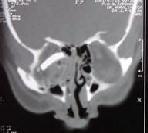
High
resolution CT
with bone window levels in addition to soft tissue and parenchymal
levels are mandatory. Anatomical discontinuities, hemorrhages, and
necrosis can be visualised. Although difficult to perform in certain
restless, confused, or unconscious patients, by varying the bone window
settings and scanning planes, it is possible to demonstrate basal skull
fractures that were previously not evident. Intracranial optic nerve
|
|
|
and chiasma can also be
imaged clearly using the present generation CT scanners.
|
Glass piece in orbit
|
|
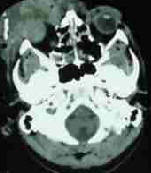
Hemorrhage in the
sphenoid and ethmoid sinus, proptosis and stretching of the optic
nerves can be documented by imaging.
Visual
Evoked Potential recording should be done as soon as possible to
have a base line and repeated every 2-3 days to assess any changes as
compared to clinical improvement. Presence of P100 wave in the VEP
indicates good prognosis. Absence of P100 wave indicates uniformly poor
visual outcome. VEP is reliable in detecting the site of lesion
particularly in patients with altered sensorium.
Electro
Retino Gram
is useful in evaluating functioning of the retina.
|
|
|
|
Burst orbit-CT
|
|
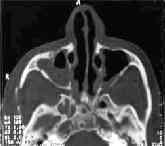
MRI
of
the orbit is useful in clearly showing the optic nerve and
chiasm. Injuries to neighboring structures such as the internal carotid
artery and pituitary gland are also well visualized.
Utrasound scan of the globe
[B-scan] will help when anterior optic nerve (anterior to the entry of
the retinal artery ) injury is suspected.
|
|
|
Management of optic nerve
injuries:
|
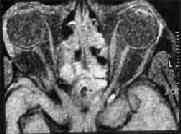
Interoccular air with medial and lateral
orbital wall fracture-CT
|
|
There is increasing interest in improving the outcome of
this potentially blinding entity. Nerve conduction defect [neuropraxia]
and damage to myelin sheath are reversible. However recovery after
damage to the retinal ganglion cells or their axons is questionable.
There is a wide variation in the extent of recovery and rate of
recovery . Axons
in the optic nerve do not regenerate after they have been
injured. This lack of axonal regenerative capacity places a
severe limitation on any therapeutic results that can be expected after
severe optic nerve injury.
|
|
|
Views are
changing.
|
Posttraumatic lens(left)
dislocation
|
|
Complete loss of vision was thought irrevocable. But
recovery in such cases has been clearly documented.
20% to 40% untreated cases may improve spontaneously
without any specific treatment.
|
|
|
Medical:
|
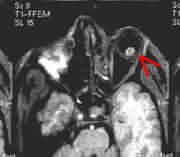
Transected right optic nerve with impinging
bone fragment-MRI
|
|
·
Methylprednisolone can reduce edema
and tissue damage ( The National Acute Spinal Cord Injury Study –
N.A.S.C.I.S II). It’s neuro protective effect has been found to
be due to it’s anti-oxidant effect. Inhibition of oxygen free radical
induced lipid peroxidation .
·
The recommended steroid protocol (Extra
cranial optic nerve decompression meeting – Boston 1993) is:·
|
|
|
|
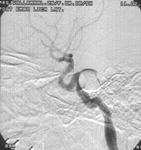
Post traumatic CCF
|
Methyl
prednisolone – 30 mg/kg IV as soon as possible
(< 8 hours)
·
followed
by – 5.4 mg/kg/hour IV in
continuous infusion for 23 hours
·
followed by
– 250 mg IV every 6 hours for 48 hours
·
followed by oral prednisolone on
tapering dosage for 15 days.
Surgery:
· The
only clear indication for operative treatment for optic nerve injury
after head trauma is where vision in the affected eye was
documented to be good initially, and progressive deterioration
occurred and thereafter and radiographs reveal a narrowed optic
canal or a bone fragment dislocated into the canal. Under these
admittedly unusual conditions, operation should be undertaken promptly,
usually within the first 48 hours after injury. Traditionally, the
operative approach of the optic canal has been via the transcranial route
with unroofing of the canal and posterior orbit. An intracranial
operation has obvious shortcomings in the acute stage after head injury
in which extensive retraction must be applied to swollen and contused
frontal and temporal lobes. For this reason, there has been a
renewed interest in acute decompression of the optic canal via the
transethmoidal, transmaxillary, and transorbital routes using
microsurgical techniques.
·
In those with orbital hemotama affecting
vision- lateral canthotomy may be considered.
Comparison
of patients treated with and without operation reveals no statistically
significant difference Results of optic canal decompression
(transethmoidal or transcranial) in many series have not been
encouraging.
Loss
of vision at the moment of impact has been considered as a contraindication
for surgery, as recovery of vision is unlikely. However, it is
impossible to determine whether the loss of vision occurred at the time
of impact or later.
Decompression.
has also been suggested when there is marginal recovery which
remains static.
Optic
nerve decompression is not recommended in unconscious patients.
Current recommendations for
the treatment of I.O.N.T.S. are as follows:
·
1.Rule out other aetiology for visual loss.
·
2.Give 30mg/kg IVmethylprednisolone load
immediately upon diagnosis.
·
3.Follow with 15mg/kg Q6hrs x 72hours
·
4.Give GI protection with H2 blockers
·
5.Obtain a CT scan to rule out bony fragments
in optic canal
·
6.Perform decompression if bony fragments are seen,
or if no improvement occurs on IV steroids after 24 hours.
The International Optic Nerve Trauma
Study group (I.O.N.T.S) observed that neither the dose nor the time
of treatment with steroids, nor time of surgical interventions affected
the visual out come. Steroid/ surgical treatment should not be the
standard procedure for the optic nerve injuries. They should be decided
on an individual basis.
B) Injury to the geniculocalcarine pathway:
The
field defect caused by this type of injury is homonymous and congruous,
but may be variable in size and location. The prognosis depends on
the primary cause and the extent of its reversibility. Infarction,
resulting from injury to the internal carotid, middle cerebral or
posterior cerebral arteries, cerebral contusion in the temporoparietal
region, or compression by a subdural or intracerebral hematoma has been
postulated as causes.
C) Cortical blindness:
This
unusual and interesting condition occurs usually in children. Often
it is the result of a mild blunt injury. There is total blindness
which is transient. It may last from a few minutes to a few hours, and
occasionally a few days. Usually it is associated with restlessness
and agitation. The pupillary reflexes are normal. Thus the
condition is easily distinguished from optic nerve and chiasmal
injuries. An EEG shows bilateral occipital slow waves. CT and
MR reveal evidence of cerebral oedema in both the occipital
regions. Recovery is usually complete. Rarely cortical
blindness may be seen in adults who have cervical injury involving the
vertebral vessels.
D) Post-traumatic delayed episodic blindness:
This
is a rare occurrence. Some weeks or months after a head injury, a
patient may report periodic sudden loss of vision occurring for a few
seconds. The episode may or may not be followed by tonic and/or
clonic convulsions associated with loss of consciousness. EEG
studies suggest that this is a paroxysmal negative visual phenomenon in
the form of an inhibitory visual seizure. CT and MR are usually
normal. The treatment is appropriate anticonvulsants.
E) Oculomotor disturbances in head injury:
Dysfunction
of the oculomotor system following trauma, may be due to injury at
different levels, varying from the cerebral cortex to the muscles in the
orbit. They can occur immediately as a result of direct
mechanical trauma or secondarily due to cerebral herniation, cavernous
sinus thrombosis, intracavernous carotid aneurysm formation, and
development of carotico-cavernous fistulas. The true prevalence of post
traumatic ocular motor nerve palsies is unclear due to difficulties in
diagnosis in unconscious patients. Orbital fractures with muscle
entrapment, contusions, and hemorrhage further complicate the
issue. Partial trochlear nerve palsies and bilateral trochlear
nerve palsies often escape attention. Abnormal erratic
wandering eye movements are present in midbrain injuries and usually
disappear when the patient regains consciousness. Focal contusions of the
midbrain may occur with or without alteration in the level of
consciousness. Various manifestations of nuclear and supra nuclear
oculomotor palsies including Parinaud’s syndrome can occur with or
without pupillary involvement, and the lesions may be unilateral or
bilateral. Occasionally, Weber’s syndrome may occur from a primary
contusional injury, but this is much more common in transtentorial
cerebral herniation. Post traumatic bilateral inter nuclear
ophthalmoplegia without any other evidence of brainstem injury has been
reported. Nystagmus is frequently seen after head injuries when either
the labyrinth or the brainstem is involved. Vertical ocular and
palatal myoclonus has also been reported after severe midbrain injury.
Contusion and laceration of the frontal cerebral cortex can present as a
supranuclear palsy of conjugate lateral gaze.
1) Oculomotor nerve injury:
3rd
nerve injury is uncommon. . The head injury is usually moderately
severe and may be either, a central frontal injury damaging the nerve in
the orbit or in the superior orbital fissure, or a temporoparietal injury
damaging the nerve against the posterior clinoid process or over the
petroclinoid ligament. There is an immediate onset of pupillary
dilatation, with no reaction to light or accommodation. The consensual
pupillary reflex in the opposite eye, with light is thrown in the
affected eye, is brisk. When the patient is fully conscious
such unilateral dilatation should not be confused with that caused
by an extradural or subdural haematoma. Regular pupillary
margin and absence of brainstem signs help to exclude other causes of
mydriasis. Sometimes a bruit may be heard in traumatic carotid
cavernous sinus fistula with a unilateral fixed dilated pupil. A
coloboma of the iris may be mistaken for a dilated pupil Traumatic
bilateral oculomotor paralysis has been reported. The prognosis is
good. Recovery starts within a few weeks and continues over a few
months. The third cranial nerve or oculomotor nerve projects from the
anterior part of the midbrain to the tentorial incisura at the level of
the posterior clinoid processes in an open V- shaped fashion. The
size of the opening in the tentorial incisura may play a part in
determining whether the nerve is injured or not. A large tentorial
opening may allow greater movement of the midbrain without damage to the
oculomotor nerve. The third nerve probably becomes damaged by a
frontal blow to the accelerating head that results in stretching and
contusion of the nerve. The exact site of damage has not been
clearly defined, but it is believed to occur most commonly at the point
where the nerve enters the dura mater at the posterior end of the
cavernous sinus. Bilateral third nerve injuries are extremely
uncommon. When the third nerve is injured at the superior orbital
fissure or in the cavernous sinus, it is often accompanied by other
cranial nerve injuries as they course through the fissure. 56%
incidence of associated optic nerve injuries, 25% incidence of associated
trigeminal nerve injuries, and 25% incidence of facial nerve
injuries when the oculomotor nerve was injured in the lateral wall of the
cavernous sinus or in the superior orbital fissure has been
reported.
The
diagnosis of oculomotor nerve injury in conscious and cooperative persons
is not difficult. In unconscious subjects, especially those with
orbital bruising and haematoma, the diagnosis is more difficult and may
escape detection if the pupil is not affected. Thus, in unconscious
patients, a good history with regard to previous oculomotor status and
the findings of the immediate post-traumatic examination, when available,
are of great help in making an early diagnosis. Such information
also helps in differentiating primary from delayed secondary oculomotor
nerve palsy.The paralysed nerve, if still in continuity, as it is in most
cases, should begin to show signs of recovery in 2 to 3 months
time. However, the phenomenon of misdirection in regeneration is
often evident. The troublesome diplopia usually subsides, but the
paralysed pupil rarely becomes normal. The pupil may not react to
light but may constrict when any one of the muscles supplied by the third
nerve contract. This amounts to a pseudo-Argyll Robertson
pupil. Due to the misdirection of the growing axons, the levator
muscle of the lid may receive fibers destined for other muscles.
When an affected individual attempts to look down, the lid becomes
elevated rather than having the globe move down.
2) Fourth nerve injury:
This
is very rare as an isolated injury. Usually it occurs in
association with third or sixth cranial nerve injury. There is no
obvious squint on inspection, but the patient complaints of diplopia on
looking downward and outward. Vertical diplopia is greater for near
objects than for distant objects. In the differential diagnosis one
has to consider fracture displacement of the orbit and injury to the
pulley of the superior oblique muscle. The fourth cranial nerve is the
last frequently injured ocular motor nerve. When involved, the
nerve is damaged by contusion or stretching as it exits the dorsal
midbrain near the anterior medullary velum. The dorsolateral
midbrain is particularly vulnerable in severe frontal blows against the
accelerating head. In this injury, the midbrain is displaced
against the postero-lateral edge of the tentorial incisura, causing
contusion, hemorrhage and damage to one or both fourth nerves.
These injuries most commonly occur in automobile and motorcycle
accidents. Lesions of the fourth nerve have to be differentiated from a
dislocation of the orbital pulley due to direct orbital trauma.
This latter injury produces a vertical diplopia mimicking a trochlear
nerve palsy but the symptoms rarely persist beyond a few weeks.The
prognosis for recovery in fourth nerve palsy is not good because the
nerve is so slender that it is often avulsed in the traumatic
process.
3) Sixth nerve injury:
This
injury is usually associated with fractures of the middle cranial
fossa. Coincident facial paralysis and deafness often occur. A
complete rupture of the nerve results in an obvious internal
squint. Partial injury, however, will produce no obvious squint and
diplopia is present only on lateral gaze. Bilateral abducens palsy
has been reported in cases of severe hyperextension injury of the
cervical spine. The mechanism suggested is an upward displacement
of the brain with avulsion of the abducens nerve under the petroclinoid
ligament. The abducens or sixth cranial nerve is injured when the head is
crushed in an antero posterior plane with resultant lateral expansion and
distortion of the skull. It may also be injured along with the
seventh and eighth cranial nerves in fractures of the petrous bone.
In such injuries, the sixth nerve is contused, stretched or severed as it
passes below the petroclinoid ligament. Vertical movement of the
brainstem during trauma may severely stretch or avulse the sixth nerve as
it leaves the pons before it enters the clival dura. Delayed
secondary paralysis of the nerve due to increased intracranial pressure
(ICP) or herniation is considered elsewhere. The abducens nerve may
also be injured at the superior orbital fissure, and this is invariably
accompanied by third and fourth cranial nerve palsies as well. The
diagnosis of abducens palsy in the unconscious patient can be made when
the affected eye fails to wander outward spontaneously, abduct when the
head is passively turned away from the side of the sixth nerve paralysis,
and abduct in response to ipsilateral cold caloric irrigation. Many
cases of abducens palsy recover spontaneously after about 4 months, a
period of time consistent with axonal regeneration.The treatment is
initially symptomatic and consists of wearing a patch over the eye to
prevent troublesome diplopia. It is customary to wait for 4 to 6
months for spontaneous regeneration to take place. If recovery does
not occur, then local muscle shortening procedures may be carried out in
the affected eye in certain situations.
F) Blow out fracture of the orbital floor:
With
increasing severity of accidents, facio maxillary injuries associated
with head injury are becoming more frequent. The condition may closely
resemble an oculomotor palsy. There is a protective ptosis.
The fracture in the floor of the orbit incarcerates the inferior oblique
muscle causing inability to move the eyeball upward. Involvement of
the inferior division of the oculomotor nerve results in a dilated
pupil. In a blow-out fracture there is infraorbital
hypoesthesia. If the conjunctiva is anaesthetized and then the
eyeball turned upwards by pulling on it with a forceps, the globe cannot
be moved because of the incarceration of the inferior oblique. In
oculomotor palsy, this manouevre will easily move the eyeball.An opaque
maxillary antrum in the skull x-ray suggests a blow-out fracture.
CT in different planes may reveal a fracture in the floor of the
orbit. In doubtful cases, positive contrast orbitography is of
value. Under local anaesthesia a needle is passed along the orbital
floor. Sometimes the fracture line may be felt by the tip of the
needle. Injection of radio-opaque dye causes an immediate leak into
the maxillary antrum.
G) Post traumatic papilledema:
Persisting
increased intracranial pressure following head injury may be due to a
variety of causes. Subacute and chronic extradural, subdural
or intracerebral haematomas form localized masses, and can be detected
and treated appropriately. Communicating hydrocephalus (due to
adhesions in the basal cisterns, or clogging of the absorption pathways
by breakdown products of the blood) and thrombosis of a major venous
sinus, especially one of the lateral sinuses can cause papilloedema
Communicating hydrocephalus responds to diuretics like acetazolamide,
hydrochlorthiazide, frusemide, glycerol and mannitol. Occasionally
surgical diversion of the CSF by a ventriculoperitoneal or lumbar
theco-peritoneal shunt may be required. Venous sinus thrombosis
also responds well to anti-oedema measures. A rare cause is traumatic
thrombosis of the carotid artery resulting in infarction and brain
swelling; “spurious papilloedema” not due to increased intracranial
pressure may occur following injury to the optic nerves and
needs to be recognized.
H) Optochiasmal arachnoiditis:
Traumatic
subarachnoid hemorrhage may rarely result in arachnoiditis involving the
chiasmatic cistern. The condition is rare. Progressive failure of
vision starts a few weeks after the head injury. Examination of the
visual fields shows a bizarre field loss. The optic discs show mild
pallor. CT shows obliteration of the chiasmatic cisterns.
Frontal craniotomy and release of adhesions should be undertaken early,
before irreversible damage to the blood supply of the optic nerves and
chiasm occurs. Good results have been reported with such surgical
treatment.
In
closed head injuries, chiasmatic injury is most commonly associated with
basal frontal fractures extending to the region of the sella turcica and
pars petrosa. . Stretch injury to the chiasm followed by
interstitial hemorrhages within the chiasm and associated contusions and
edema have been postulated. Post-traumatic chiasmal lesions may have
bitemporal hemianopsia with or without macular sparing, depending
on whether the macular fibers have escaped injury In the unconscious
patient this can be demonstrated by Wernicke’s hemianopic pupillary
reaction.
It
is essential that the ophthalmologist be aware of clinical
manifestations of injuries in and around the globe of the eye. It
should never be forgotten that rarely, even if conscious level is well
preserved a compressive sub acute or chronic extra dural or sub dural
hematoma may manifest with neuro ophthalmic manifestations. Imaging
studies and neurosurgical consultation is mandatory.
|