|
The term
'Diplopia' is derived from the Greek; diplous meaning double
and ops meaning eye. Diplopia causes significant difficulty
with depth perception and orientation of objects. Adults are capable
of expressing this symptom unlike children; in addition, in children
the image from the defective eye is suppressed due to the immature
visual system.
There is no
information available regarding its epidemiology.
Ocular media abnormalities, such as corneal scarring,
cataract, vitreous abnormalities, and retinal conditions result in
monocular diplopia.
A number of pathological processes can cause ocular
nerve (3rd, 4th, & 6th cranial nerves) palsies produce binocular
diplopia, encountered in neurological practice.
THIRD
[OCULOMOTOR] NERVE:
Neuro-Anatomy: This nerve
innervates by the Superior division - the Levator palpebrae
superioris and the Superior rectus muscle and
by the
Inferior division - the Inferior rectus, the Medial rectus, the
Inferior oblique, the Sphincter pupillae, and the Ciliary muscle.
The nuclear
complex of the third (oculomotor) nerve is situated in the mid-brain
at the level of the superior colliculus, inferior to the sylvian
aqueduct. It is composed of the following paired and unpaired
subnuclei:
·
The levator subnucleus is an unpaired caudal midline structure which
innervate both levator muscles. Lesions confined to this area will
therefore give rise to bilateral ptosis.
·
The superior rectus subnuclei are paired and innervate their
respective contralateral superior rectus muscles.
·
The medial rectus, the inferior rectus and the inferior oblique
subnuclei are paired and innervate their corresponding ipsilateral
muscles.
Lesions
involving purely the third nerve nuclear complex are relatively
uncommon.
The
most frequent causes are vascular disease, demyelination, primary
tumors, and metastases.
Lesions
involving the entire nucleus cause an ipsilateral third nerve
palsy with ipsilateral sparing and contralateral weakness of
elevation.
Lesions
involving the paired medial rectus subnuclei cause a wall-eyed
bilateral internuclear ophthalmoplegia (WEBINO) characterized by
defective convergence and adduction.
The
fasciculus consists of efferent fibers which pass from the third
nerve nucleus through the red nucleus and the medial aspect of the
cerebral peduncle. They then emerge from the mid-brain and pass into
the interpeduncular space. Benedikt's syndrome involves the
fasciculus as it passes through the red nucleus. It is characterized
by an ipsilateral third nerve palsy and a contralateral hemitremor.
Weber's
syndrome involves the fasciculus as it passes through the cerebral
peduncle. It is characterized by an ipsilateral third nerve palsy and
a contralateral hemiparesis.
The
basilar part starts as a series of 'rootlets' which leave the
mid-brain before coalescing to form the main trunk. The nerve then
passes between the posterior cerebral artery and the superior
cerebellar artery, running lateral to and parallel with the posterior
communicating artery because the nerve traverses the base of the
skull unaccompanied by any other cranial nerves, isolated third nerve
palsies are frequently basilar.
|
The following two are important causes:
1. Aneurysms at
the junction of the posterior communicating artery and the internal
carotid artery.
2. Extradural
hematomas, which may cause a tentorial pressure cone with downward
herniation of the temporal lobe. This compresses the third nerve as
it passes over the tentorial edge initially causing a fixed dilated
pupil followed by a total third nerve palsy.
|
|
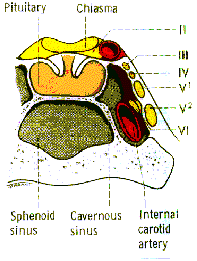
The
intracavernous part enters the cavernous sinus by piercing the dura
just lateral to the posterior clinoid process. Within the cavernous
sinus, the third nerve runs in the lateral wall and occupies a
superior position above the fourth nerve. In the anterior part of the
cavernous sinus, the nerve divides into superior and inferior
branches which enter the orbit through the superior orbital fissure
within the annulus of Zinn. The following are important causes of
intracavernous third nerve palsies: Diabetes which may cause a
vascular palsy.
Pituitary
apoplexy which may cause a third nerve palsy as a result of
hemorrhagic infarction of a pituitary adenoma (e.g after childbirth),
with lateral extension into the cavernous sinus.
Intercavernous
lesions such as aneurysms, meningiomas, carotid-cavernous fistulae
and Granulomatous inflammation (Tolosa-Hunt syndrome) may all cause
third nerve palsies.
Because
of its close proximity to other cranial nerves, intracavernous third
nerve palsies are usually associated with involvement of the fourth
and sixth nerves and the first division of the trigeminal nerve; the
pupil is frequently spared.
The
intraorbital part divides into the following:
The superior
division which innervates the levator and superior rectus muscles.
The inferior
division which innervates the medial rectus, the inferior rectus and
the inferior oblique muscles. The inferior branch of the third nerve
within the orbit also contains the parasympathetic fibers from the
Edinger-Westphal subnucleus, which innervate the sphincter pupillae
and the ciliary muscle. Lesions of the inferior division are
characterized by limited adduction and depression, and a dilated
pupil.
The
main causes of both superior and inferior division palsies are trauma
and vascular disease.
Pupillomotor
fibers: The location of these
parasympathetic fibers in the trunk of the third nerve is clinically
very important. Between the brain stem and the cavernous sinus, the
pupillary fibers are located superficially in the superior median
part of the nerve. They derive their blood supply from the pial blood
vessels, whereas the main trunk of the third nerve is supplied by the
vasa nervosum. The presence or absence of pupillary involvement is of
great importance because it frequently differentiates a so-called
'surgical' from a 'medical' lesion.
Surgical
lesions such as aneurysms, trauma and uncal herniation
characteristically involve the pupil by compressing the pial blood
vessels and the superficially located pupillary fibers.
Medical
lesions such as hypertension and diabetes usually spare the pupil.
This is because the microangipathy associated with medical lesions
involves the vasa nervosum, causing neural infarction of the main
trunk of the nerve, but sparing the superficial pupillary fibers.
Clinical features of
third (Oculomotor) nerve palsy:
·
Ptosis due to weakness of levator
·
Eyeball is divergent and slightly downwards due to
unopposed action of the lateral rectus (N VI)
and superior oblique (N IV) muscles.
·
Intorsion of the eyeball on attempted down gaze, due to action of
superior oblique muscle.
·
Ocular movements are restricted in all directions [elevation,
depression & adduction] except outwards (due to lateral rectus)
·
Pupil is dilated, and does not constrict to light or convergence.
Difficulty for small print is present
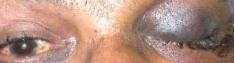
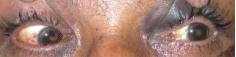
POST TRAUMATIC LEFT OCULOMOTOR NERVE PALSY
|
|
|
|
Complete ptosis with ecchymoses
|
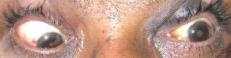
Left exotropia
|
|
|
|
|
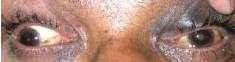
Adduction Restricted
|
Abduction Normal
|
|

|
|
|
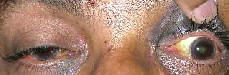
Elevation restricted
|
Depression restricted
|
Aberrant
regeneration may occasionally follow acute traumatic and aneurysmal,
but not vascular, third nerve palsies. The bizarre defects in ocular
motility, such as elevation of the upper eyelid on attempted
adduction or depression, are caused by misdirection of sprouting
axons reinnervating the wrong extraocular muscle. The pupil may also
be involved in some cases.
Causes of isolated third
nerve palsy:
In order of
frequency the following are causes of an isolated third nerve palsy:
Idiopathic :
about 25% have no known cause.
Vascular
disease such as hypertension and diabetes are the most common causes
of a pupil-sparing third nerve palsy. All patients should therefore
have blood pressure measurement and urine analysis. In most cases
recovery occurs within 3 months. Diabetic third nerve palsies are
often associated with periobital pain and are occasionally the
presenting feature of diabetes. The presence of pain is not helpful
in differentiating between an aneurysmal and a diabetic third nerve
palsy because both are frequently accompanied by pain.
Trauma is
also a common cause. However, the development of a third nerve palsy
following relatively trivial head trauma, not associated with loss of
consciousness, should alert the clinician to the possibility of an
associated basal intracranial tumour which has caused the nerve trunk
to be stretched and tethered.
An aneurysm
at the junction of the posterior communicating artery with the
internal carotid is a very important cause of an isolated painful
third nerve palsy with involvement of the pupil.
Miscellaneous
uncommon causes include tumors, vasculitis associated with collagen
vascular disorder and syphilis.
As with all
ocular motor nerve palsies, surgical treatment should be contemplated
only after all spontaneous improvement has ceased. This is usually
not earlier than 6 months from the date of onset.
FOURTH [TROCHLEAR] NERVE:
Neuro-anatomy:The fourth nerve differs from
other cranial nerves as follows:
It is
the only cranial nerve to emerge from the dorsal aspect of the brain.
It is
the only crossed cranial nerve; this means that the fourth nerve
nucleus innervates the contralateral superior oblique muscle.
It is
the longest and most slender of all cranial nerves.
The
nucleus of the fourth nerve is located at the level of the inferior
colliculus beneath the sylvian aqueduct. It is caudal to, and
continuous with, the third nerve nuclear complex.
The
fasciculus consists of axons which curve around the aqueduct and
decussate completely in the anterior medullary velum.
The trunk
leaves the brain stem on the dorsal surface, just caudal to the
inferior colliculus. It then curves forward around the brain stem,
runs beneath the free edge of the tentorium, and (like the third
nerve) passes between the posterior cerebral artery and the superior
cerebellar artery. It then pierces the dura and enters the cavernous
sinus.
The
intracavernous part runs laterally and inferiorly to the third nerve
and above the first division of the fifth. In the anterior part of
the cavernous sinus it rises and passes through the superior orbital
fissure above the annulus of Zinn.
The
intraorbit part innervates the superior oblique muscle.
Clinical
features of fourth nerve palsy:
The
clinical features of a nuclear, fascicular and a peripheral fourth
nerve palsy are clinically indistinguishable.
·
Hyper deviation (involved eye is higher) as a result of
weakness of the superior oblique muscle. This is more obvious when
the head is titled to the ipsilateral shoulder (Bielschowsky’s head
tilt test).
·
Excyclotorsion which is compensated for by a head tilt to the
opposite shoulder.
·
Limited depression in adduction.
· Diplopia
which is vertical and worse on looking down. In order to avoid
diplopia the patient may adopt an abnormal head posture with a
downward head tilt and a face turn to the opposite
side.·
Post Traumatic Right Trochlear Nerve Palsy
|

|

|

|
|
Right hyper tropia in primary gaze with head
straight.
|
Eyes aligned with head tilt to the left side.
|
Post operative-Eyes aligned with head straight.
(Surgery done after four to six months to the right inferior oblique
and left inferior rectus in two stages.)
|
Causes
of isolated fourth nerve palsy:
1.Congenital
lesions are frequent, though symptoms may not develop until adult
life. Abnormal head posture [ocular torticollis]in old photographs
when available can be of help.
2.Trauma
often causes bilateral palsies as the slender nerves are vulnerable
as they decussate in the anterior medullary velum through impact with
the tentorial edge.
3.Vascular
lesions are common but aneurysms and tumors are rare.
Medical
investigations are the same as for a pupil sparing third nerve
palsy.
SIXTH
[ABDUCENS] NERVE
Neuro-anatomy: The nucleus
of the sixth (abducens) nerve lies in the midpoint of the pons, inferior
to the floor of the fourth ventricle, where it is closely related to
the fasciculus of the seventh nerve. An isolated sixth nerve palsy is
therefore never nuclear in origin.
A
lesion in and around the sixth nerve nucleus causes the following
signs:
·
Failure of horizontal gaze towards the side of the lesion resulting
from involvement of the horizontal gaze centre in the pontine
paramedian reticular formation (PPRF).
·
Ipsilateral weakness in abduction as a result involvement of the
nucleus.
·
Ipsilateral facial nerve palsy caused by concomitant involvement of
the facial fasciculus which is also common.
The fasciculus
consists of emerging fibres which pass ventrally to leave the brain
stem at the pontomedullary junction, just lateral to the pyramidal
prominence.
Foville’s
syndrome involves the fasciculus as it passes through the PPRF and is
characterized by the following ipsilateral signs: sixth nerve palsy
combined with a gaze palsy, facial weakness caused by damage to the
facial nucleus or fasciculus, facial analgesia from involvement of
the sensory portion of the fifth nerve, Horner’s syndrome and deafness.
Millard-Gubler syndrome involves the fasciculus as it passes through
the pyramidal tract and is characterized by ipsilateral sixth nerve
palsy, contralateral hemiplegia and variable number of signs of a
dorsal pontine lesion.
The basilar
part leaves the mid-brain at the pontomedullary function and
enters the prepontine basilar cistern. It then passes upwards close
to the base of the pons and is crossed by the anterior inferior
cerebellar artery. It pierces the dura below the posterior clinoids
and angels forwards over the tip of the petrous bone, passing through
or around the inferior petrosal sinus, through Dorello’s canal (under
the petroclinoid ligament) to enter the cavernous sinus.
The
following are important causes which may damage the basilar
portion of the nerve.
1.
An acoustic neuroma may damage the sixth nerve as it leaves the
mid-brain at the pontomedullary junction. It should be emphasized
that the first symptom of an acoustic neuroma is hearing loss and the
first sign is a diminished corneal sensitivity. It is therefore
very important to test hearing and corneal sensation in all patients
with sixth nerve palsy.
2.
A nasopharyngeal tumor may invade the skull and its foramina and
damage the nerve during its basilar course.
3.
Raised intracranial pressure associated with posterior fossa tumors
or benign intracranial hypertension (pseudotumor cerebri) may cause a
downward displacement of the brain stem: This may stretch the sixth
nerve over the petrous tip between its point of emergence from the
brain stem and its dural attachment on the clivus. In this situation,
the sixth nerve palsy, which may be bilateral, is a false localizing
sign.
4.
A basal skull fractures may cause both unilateral and bilateral
palsies.
The
intracavernous part runs forwards below the third and fourth nerves,
as well as the first division of the fifth. Although the other nerves
are protected within the wall of the sinus, the sixth is most
medially situated and runs through the middle of the sinus in close
relation to the internal carotid artery. It is therefore more prone
to damage than the other nerves. Occasionally, an intracavernous
sixth nerve palsy is accompanied by a postganglionic Horner’s
syndrome because in it’s intracavernous course the sixth nerve is
joined by the sympathetic branches from the paracarotid plexus.
The causes of intracavernous sixth nerve and third nerve lesions are
similar.
The
intraorbital part enters the orbit through the superior orbital
fissure within the annulus of Zinn to innervate the lateral rectus
muscle.
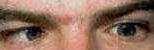
Clinical features of
sixth nerve palsy:
|

|

|
|
|
Left esotrpoia
|
Normal adduction of left eye
|
Abduction restricted in the left eye
|
Defective abduction is caused by weakness of the lateral rectus
with normal adduction.
In the primary position, there is a convergent strabismus as a result
of the unopposed action of the medial rectus.
The
face is turned into the field of action of the paralyzed muscle to
minimize diplopia, so that the eyes are turned away from the field of
action of the paralyzed muscle. For example, a patient with a left
sixth nerve palsy will turn the face to the left.
Horizontal diplopia is worse in the field of action of the paralyzed
muscle and least away from its field of action.
Most of the causes of an isolated sixth nerve palsy have already been
mentioned, but, in contrast to third nerve palsy, aneurysms rarely
cause a sixth nerve palsy. Vascular causes (especially diabetes and
hypertension) are, however, common.
PARALYTIC SQUINT
It
is the mis-alignment of the visual axes as a result of paresis, or
paralysis of one or more extra-ocular muscles. It is characterized by
impaired movement in the field of action of the muscle or
muscles, and thus the angle of deviation varies in different
directions of gaze.
CLINICAL FEATURES:
Binocular
diplopia
An
object appears double with both eyes remain open. This occurs when
the image of an object does not fall on the corresponding points of
the retina of the both eyes. Image of an object falls on the fovea of
one eye, and on the extra foveal area of the opposite eye.
Causes
1.
Paralysis or paresis of the extra-ocular muscles (commonest)
2.
Displacement of the eyeball, by a space occupying lesion in the
orbit, by fracture of orbital wall or by pressure of fingers.
3.
Mechanical restriction of the movements of the globe e.g. pterygium,
symblepharon, thyroid ophthalmopathy etc.
4.
Deviation of rays of light in one eye, as in decentered spectacles.
5.
Disparity of image size between two eyes, as in acquired high
aniso-metropia.
In diplopia one image is distinct (true image), and the other is
indistinct (false image). Binocular diplopia disappears when one eye
is closed. Depending on the position of the false image in relation
to midline, binocular diplopia may be uncrossed or crossed.
·
False orientation of the object: object is projected too far in the
direction of paralyzed muscle, due to increase in secondary
deviation.
·
Vertigo and nausea: They are partly due to diplopia, and partly due
to false orientation.
·
Secondary angle of deviation is more than the primary deviation.
·
Restriction of ocular movements in the direction of action of
paralyzed muscle.
·
Compensatory head posture:
In
paralytic squint to neutralize diplopia, the chin may be elevated or
depressed.
The
face turned to right or left side.
The
head tilted to the right or left shoulder (ocular torticollis).
This
head posture, is to neutralize the angle of deviation, or to
separate the images maximally, so as to avoid
diplopia.
In
paralysis of horizontal rectus muscle, the face is turned to field of
action of the paralyzed muscle, but the head is not tilted. As, in
right lateral rectus palsy, the patient keeps his face turned to the
right.
In
case of cyclo-vertical muscle palsy, it is more complicated, and less
valuable diagnostically. As in superior oblique palsy, the head is
tilted on the side of the normal eye, the face is turned opposite to
normal side, and the chin is depressed.
·
Visual acuity is normal in both eyes, and there is no
amblyopia.
Different types of ocular paralysis:
Total
ophthalmoplegia: It means involvement of both extrinsic and intrinsic
muscles of the eyeball. In unilateral cases, the lesion is in the
cavernous sinus, or in the superior orbital fissure, and in bilateral
cases, the lesion is widespread in the brain-stem (due to
inflammatory cause).
Clinical signs:
Ptosis.
·
The eyeball is slightly proptosed and divergent (due to anantomical
positon of rest).
·
No movement of the eyeball in any direction
·
Fixed dilated pupil (no reaction to light, accommodation and
convergence).
·
Total loss of accommodation.
External
ophthalmoplegia: It is due to paralysis of extrinsic muscles which
includes six extra-ocular muscles and the levator. It is due to
nuclear lesion without affecting the Edinger-Westphal nucleus, which
supplies the intrinsic muscles.
Signs
are same as total ophthalmoplegia except, that the pupillary reaction
and accommodation are normal.
Investigations
of paralytic squint:
History,
careful complete clinical examination and appropriate investigations
including radio imaging to identify the causative factor
Diplopia
Charting/Hess Lee’s Screening initially to identify the eye muscle
affected and later at four to six weeks to know about the progress.
Measurement
of angle of deviation by synoptophore or prism bar.
Forced
duction test (FDT): This test is used to differentiate defective
ocular movements due to physical restriction, from a muscle
paralysis.
After
topical anesthesia, the insertion of the affected muscle is grasped
with fixation forceps, and gently attempted to rotate the eyeball in
the field of action of weak muscle. FDT-‘Positve’ means, it is
difficult to move the globe with the forceps (e.g., contracture of
muscle as in thyroid myopathy, trapped muscle in orbital floor
fracture etc.)
FDT
is ‘negative’ in case of muscle paralysis.
Treatment
of paralytic squint:
Treatment
must be directed to the cause of paralysis.
Ischemic lesion can resolve spontaneously
For the relief of diplopia: [if present only in the practical field
of fixation i.e in the straight and down gazes]
Occlusion of affected eye temporarily.
Suitable prism correction for minor diplopia.
Observation for at least 6 months, so that maximum amount of
spontaneous recovery could take place.
Recession of contra-lateral synergist may be done for the nerve
palsy. Alternately, various type of muscle transposition operations
may be undertaken.
Botulinum toxin injection – to treat the antagonist muscle to prevent
its contracture.
CRANIAL NERVE SYNDROMES:
These
syndromes were of help for topo graphical localization prior to radio
imaging techniques.
WEBER
Ipsilateral third nerve palsy
Contralaterl hemiparesis
BENEDICT
Ipsilateral third nerve palsy
Contralateral hemi tremor
MILLARD- GUBLAR
Ipsilateralsixth nerve palsy
Ipsilateral seventh nerve
Contra lateral hemiplegia
FOVILLE
Ipsilateral sixth nerve palsy
Gaze palsy
Facial weakness
Facial analgesia
Horner’s syndrome
Deafness
GRADENIGO
Petrositis
TOLOSA HUNT
Painful ophthalmoplegia due to granulomatous lesion in
cavernous sinus
|